Picture this: it’s 2am, your child can barely breathe. You call an ambulance, rush to the hospital, and somehow make it through the night. Then morning comes — and that’s when someone calmly asks you for ¥100,000 in cash. Before they process your admission.
That was me, in December 2025, standing at a hospital admissions counter in Japan the morning after my son’s emergency — exhausted, still running on adrenaline — being told that without health insurance, the estimated bill for a five-day stay could exceed ¥1,000,000.
I know. Wild, right?
Here’s the thing — I’m Japanese. I grew up in Japan, and I even worked at a GP-style clinic (内科小児科クリニック) before moving to New Zealand a decade ago. I thought I knew the system. But after ten years of navigating New Zealand’s public healthcare as a mum to a son with a complex medical history, going back to a Japanese hospital felt like landing in a parallel universe.If you’re travelling to Japan, living there, or just curious about how things work — this article is for you. I’m not a medical professional giving advice. I’m just a Japanese woman in New Zealand who has, at this point, experienced everything the healthcare system has to offer on both sides of the world: consultations, hospitalisations, surgeries, and yes — ambulances.
In this article, I’ll walk you through three key areas:
- Seeing a doctor (clinics vs. hospitals)
- Being hospitalised
- Calling an ambulance
No textbook stuff. Just honest, first-hand comparison — with a few jaw-dropping moments along the way.
🩺 Quick Take
- Clinics in Japan are walk-in friendly with same-day access — a huge contrast to appointment-only GPs in NZ and much of the Western world.
- Hospitalisation involves upfront paperwork, cash deposits, and longer stays — but the food is genuinely excellent.
- Ambulances are free in Japan and impressively fast. In NZ (and many Western countries), they’re not — which changes how people decide whether to call one.
What’s the Difference Between a Clinic and a Hospital in Japan?
Think of it like this: in New Zealand (and much of Europe and North America), your first point of contact for non-emergency healthcare is your GP — General Practitioner. You book an appointment, sometimes days or even weeks in advance, and see the same doctor who knows your history.
In Japan, the equivalent is the クリニック/診療所 (clinic) — often a small, specialised practice like an internal medicine and paediatric clinic (内科小児科クリニック), which is exactly where I worked before leaving Japan. You can see a doctor for everything from a cold to a check-up.
The big difference? Appointments are often optional.
While fully appointment-based clinics do exist in Japan, they’re genuinely the minority. Most clinics operate on a walk-in basis, or a hybrid system that’s distinctly Japanese:
- 順番予約 (Queue-based reservation): You “book” your spot in line — either in person or via app — and come back when it’s your turn. Think of it like getting a number at a deli counter, except you can track your position on your phone from a café down the street.
- 時間帯予約 (Time-slot reservation): You book a 30-minute or one-hour window, but multiple patients are slotted into the same block. Your actual order within that window? First come, first served upon arrival.
The Upside (And It’s a Big One)
The beauty of the Japanese clinic system is that when you feel unwell, you can actually be seen that day. There’s a wait — sometimes a long one — but you don’t have to suffer through the weekend hoping things improve before Monday’s first available appointment slot. As someone who has genuinely cried on the phone trying to get a same-week GP appointment in NZ, I cannot overstate how refreshing this is.
When It Gets Complicated: Hospitals
If your clinic doctor decides you need specialist care or further investigation, they’ll refer you to a 病院 (hospital). And here’s where the pace dramatically slows down.
Hospitals in Japan — for non-emergency cases — run on full appointment systems. And yet, inexplicably, the wait times can be extraordinary. A 10am appointment that doesn’t result in you actually seeing a doctor until noon? Completely normal. If you have a hospital appointment in Japan, bring a book. Bring snacks. Bring patience.
Being Hospitalised in Japan: What Actually Happens
This is where Japan and New Zealand diverge most dramatically. And I say that as someone who has shepherded my son through multiple hospitalisations in both countries.
My son was born extremely premature — a super low birth weight baby — and has a medical history that reads like a small novel. Hospitalisations happen in our family. I am, unfortunately, quite practised at this.
In New Zealand: Casual (Almost Too Casual)
In NZ’s public hospital system, admission paperwork is minimal. Because it’s publicly funded, there’s no billing process, no upfront payment, nothing financial to navigate. You’re triaged, admitted if needed, and eventually discharged when you’re well enough to manage at home. The system errs on the side of getting you home sooner rather than later — and I’ll be honest, there have been times where I felt we were discharged a little too soon for comfort.
In Japan: Thorough (Almost Too Thorough)
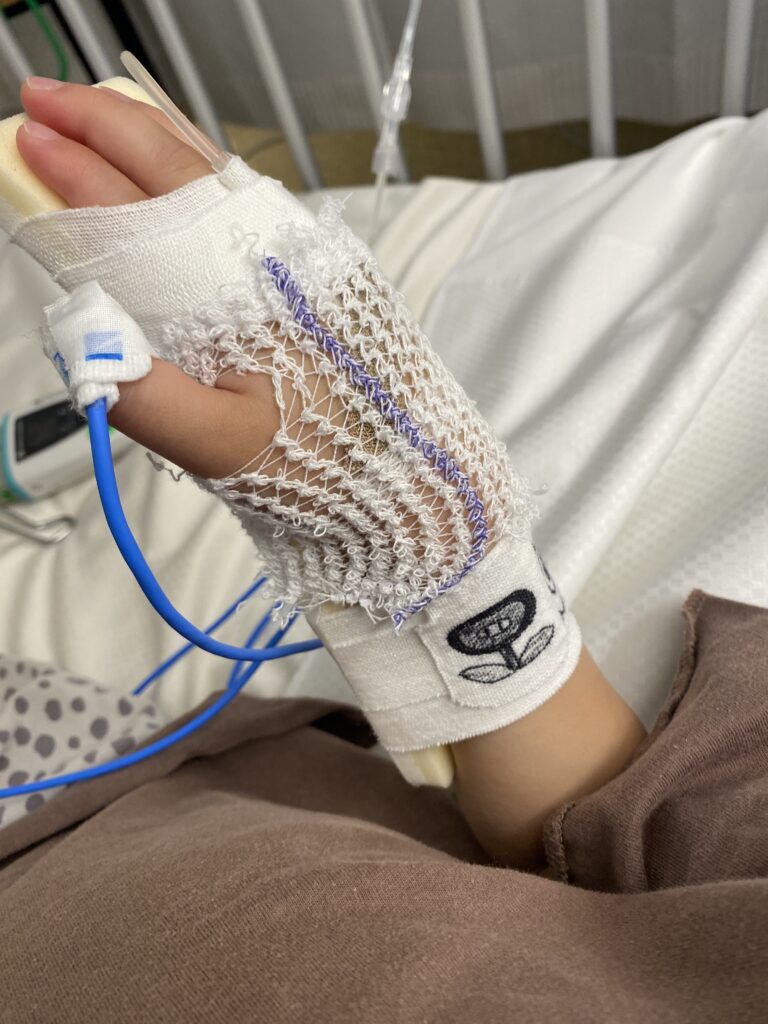
In December 2025, during a visit back to Japan, my son had a severe asthma attack in the middle of the night and was taken by ambulance to a private hospital. That night, we were absorbed entirely into emergency care — there was no paperwork, no financial conversation, nothing like that. It was only the next morning, once the reception desk opened, that I was directed to the 入院受付 (inpatient admissions counter) to complete the following:
- Submit the 保険証 (health insurance card)
- Pay an upfront deposit (頭金) — in our case, ¥100,000 in cash for insured patients
- Sign various forms and consent documents
The staff were kind about it, and I want to be clear: this isn’t unusual or unreasonable by Japanese standards. But if you’re a traveller without Japanese health insurance? The deposit for an uninsured patient was quoted as the full estimated cost — and for a projected five-day stay, that figure was a minimum of ¥700,000, potentially exceeding ¥1,000,000.
I stood there, still exhausted from the night before, doing very rapid mental arithmetic.
A few things worth knowing:
- The deposit rules vary by hospital — always ask upfront.
- If you have travel insurance, it may cover this, but you’ll likely need to pay first and claim later.
- Health insurance card (保険証) is essential for residents. Visitors should have comprehensive travel insurance. Full stop.
📋 Japan 101: What Is the 保険証 (Health Insurance Card)?
If you live and work in Japan, you’re enrolled in the national health insurance system (国民健康保険, Kokumin Kenko Hoken) and issued a 保険証 (hoken-sho) — a small card that serves as proof of your coverage. Present it at any clinic or hospital, and your medical costs are typically covered at 70%, with the remaining 30% paid out of pocket.
For tourists and short-term visitors, the 保険証 doesn’t apply — you won’t have one. This is why comprehensive travel insurance is so important. Without it, you’re looking at full out-of-pocket costs, which (as you’ve just read) can be eye-watering. Check that your policy covers emergency hospitalisation and medical evacuation before you travel. It’s the kind of thing you hope you’ll never need — until suddenly you do.
Discharge: Cured vs. Stable
Another notable difference: in NZ, “good enough to go home” is the discharge threshold. In Japan, the tendency is to keep patients until they are considered fully recovered — treatment complete, not just stable.
Honestly? My feelings on this are genuinely mixed. Part of me appreciated the thoroughness — knowing we weren’t being sent home before the doctors were truly satisfied felt reassuring. But another part of me, by day three or four, was quietly counting the days and wondering if we could please just go home and recover in our own space. There’s something about being stuck in a hospital room, even a perfectly good one, that makes you desperate for your own bed. I imagine anyone who’s spent time in hospital — anywhere in the world — knows that feeling. So: thorough, yes. But also, as a parent, you sometimes find yourself in the strange position of hoping your child gets better quickly enough to leave, while simultaneously being grateful that the bar for “better enough” is set so high.
The Food: Japan Wins, No Contest
I cannot write about Japanese hospitalisation without mentioning the food, because it was genuinely one of the most delightful surprises.
Warm, balanced meals. A small snack in the afternoon. Tea. Actual hot tea, in a hospital.
When I was hospitalised in NZ (yes, I’ve had my turn too), the meals were… fine? Nutritionally questionable, heavy on processed carbs, notably short on vegetables and fruit. We ended up bringing food from home most days. The NZ hospital food was free, which I appreciate — but the contrast was stark.
In Japan, meals are charged separately (自費) and included in your hospital bill. But we’re talking a few hundred yen per day. For food that was thoughtfully prepared and genuinely good. My son finished every single meal and then enthusiastically told me about it afterwards. He even discovered a new favourite Japanese dish during that stay, which felt like the most unexpected silver lining of the whole ordeal. I’ve never seen a child look so pleased about hospital food.


Calling an Ambulance in Japan
Let’s get straight to the most surprising part: in Japan, ambulances are free.
Not discounted. Not means-tested. Free.
In New Zealand, calling an ambulance costs money — enough that many people (myself included) think twice about whether to call one or just drive to the emergency department ourselves. When the roads are clear and the patient is stable enough, we often choose the car.
In Japan, ambulances are operated as a public administrative service (公的行政サービス), the philosophy being that in a genuine emergency, nobody should be delayed by financial considerations.
The Night I Called 119
Back to that December night. My son — breathing difficulties worsening fast, history that made it complicated — and we had no car in Japan. I called 119 (Japan’s equivalent of 111 in NZ or 999 in the UK).
Here’s what happened:
- The dispatcher first confirms: emergency (救急) or fire (消防)? Worth knowing before you panic-dial.
- Once confirmed as a medical emergency, they ask about the patient, the caller, and what’s happening.
- If the situation sounds serious, they dispatch the ambulance while still on the line with you. In our case, the ambulance arrived in approximately 5 minutes from when I called.
- Inside the ambulance, the paramedics conduct an initial triage and take a verbal medical history.
- They then call ahead to find an available emergency department — working through a priority list of hospitals in the area, one by one. Our first choice was full. The second accepted us. (Luckily, it turned out to be near my parents’ home.)
My biggest practical tip from this experience:
Keep a medical summary on your phone. Mine had my son’s full diagnosis history, hospitalisations, medications, and treatment protocols — in both English and Japanese. I showed the Japanese version to the paramedics and the receiving doctors, and it saved an enormous amount of time and confusion. If you’re travelling to Japan with any kind of medical complexity, prepare a summary in advance and use AI translation into Japanese if needed.
One more thing: you’ll need internet for that AI translation. Japan’s WiFi situation is… patchy. Our hospital happened to have reliable free WiFi, but don’t count on it everywhere. (I’ve written more about navigating WiFi in Japan here.)
Practical Tips: Navigating Japanese Healthcare as a Non-Resident
- At a clinic: Walk-ins are usually fine, but it’s worth checking the clinic’s website first if you can — many clinics now have an online reservation system where you can check wait times or book your spot in the queue before you arrive. If there’s no website, or no online system, simply walking in and waiting is usually perfectly fine. Either way, expect a wait; bring something to do.
- At a hospital: Bring your health insurance card (保険証). For non-residents, bring your travel insurance details and be prepared to pay upfront and claim later.
- For hospitalisation: Ask upfront about the deposit policy. Have access to cash or an international card. Pack like you might be there a while.
- For emergencies: The number is 119. Ambulances are free, and the response time (in urban areas) is genuinely impressive.
- Prepare a medical summary: Even if it’s just allergies and a list of regular medications — have it written down, and consider a Japanese translation.
- Travel insurance: Not optional. Please, just get it.
Final Thoughts
Healthcare is one of those things you never really think about until you need it — and then suddenly it’s all you can think about.
Japan’s medical system has a lot going for it: same-day clinic access, thorough treatment, incredibly fast ambulances, and hospital food that puts many restaurants to shame. It also has things that can catch you off guard: cash deposit requirements, marathon wait times at hospitals despite having an appointment, and a system that really, truly assumes you have that insurance card.
Going in with some knowledge makes all the difference. And honestly? After everything we’ve been through — the midnight ambulance ride, the ¥100,000 deposit, the surprisingly good hospital curry — I’ve come away with a deep respect for how Japan approaches care.
I hope this helps you feel a little more prepared, wherever your Japan adventures take you.
Have you ever had to navigate healthcare in a foreign country? I’d love to hear your story — drop it in the comments below. And if this article helped, please share it with a friend who’s heading to Japan — it might just save them a midnight panic.





